Long-term disability (LTD) benefits are paid out by insurance companies according to the policy purchased by a worker, their union/association or their employer, and each has specific rules regarding how you qualify for long-term disability benefits.
The general rule of thumb is that a diagnosed medical condition that prevents you from carrying out the main duties of your work will qualify you for long-term disability – unless your condition is explicitly excluded in the wording of the policy or, like in the majority of LTD policies, it is a pre-existing condition.
Learn what medical conditions typically qualify for long-term disability, how to apply and how one of the more experienced disability lawyers in Toronto can still get you LTD benefits if your claim is denied, as they routinely are.
Disclaimer: The information in this guide and everywhere else on this website is for general information only and is not intended to provide legal advice of any kind. No lawyer-client relationship is created by accessing or otherwise using Ertl Lawyers’ website or by communicating with a lawyer or staff member. Please contact the leaders in employment and disability law at Ertl Lawyers if you need legal advice. We’re more than happy to speak with you.
The Basics of Qualifying for Long-Term Disability
According to the last Canadian Survey on Disability (2017), approximately one in five Canadians over the age of 15 has one or more disabilities that limit their daily activities. Data from the next Survey is scheduled to be released in December of 2023.
Long-term disability insurance is intended to provide workers who are injured in an accident or who develop a disabling medical condition with a portion of their earnings in regular instalments. The amount of the LTD benefits and how frequently they are paid out depend on the policy. Benefits are typically paid monthly and can be anywhere from 50 – 80% of your regular wages.
How Serious Does My Medical Condition Have to be to Qualify for Long-Term Disability?
Aside from excluded and pre-existing conditions, you can qualify for long-term disability benefits if your medical condition meets the definition of what is commonly referred to as a “total disability.” A total disability does not mean that you are completely incapacitated or have suffered a catastrophic injury. There are two classifications of a total disability:
- Being totally disabled from your “own occupation.” This usually means that you are no longer able to perform the regular, core functions of the position you held prior to suffering from your disability.
- A total disability that prevents you from working in “any occupation.” This means that you are no longer able to perform not just your own work but work that you may already be reasonably suited to perform given your experience, training or education, or that you might be able to perform with proper training.
When you apply for LTD benefits, your policy may use either classification as the threshold for qualification. However, if your LTD insurance covers an own occupation disability, your policy more than likely states that after two years, you must be totally disabled under their any occupation definition, or your benefits will be terminated as you will no longer qualify for LTD benefits.
Speak to a disability lawyer as soon as possible if you receive this notice. LTD lawyers often challenge this change in definition and can force the insurance company to continue paying benefits.
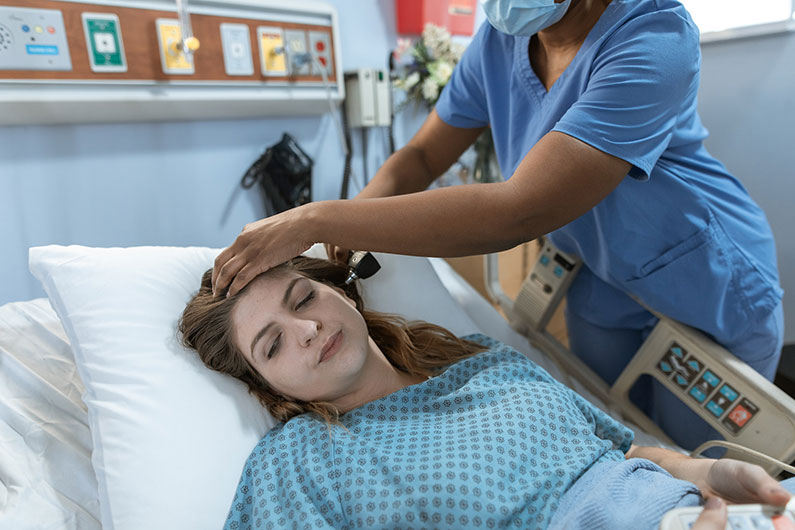
What Kind of Medical Conditions Usually Qualify for Long-Term Disability Benefits?
It’s important to note that your illness or injury does not have to be work-related for you to qualify for LTD benefits.
In fact, unless your work is in an exempted industry, your employer is required to carry Workplace Safety and Insurance Board (WSIB) coverage. If you are injured at work or because of your work, WSIB can pay for lost wages and medical expenses if you qualify.
Some of the more common medical conditions that qualify for long-term disability benefits include:
- Chronic conditions like Chronic Fatigue & Chronic Pain Syndrome.
- Back, muscle and joint disorders such as Rheumatoid Arthritis, Fibromyalgia and Osteoarthritis.
- Mental illnesses including Depression, PTSD and Anxiety.
- Cardiovascular conditions such as Heart Disease & Stroke.
- Cancers and tumours.
- Spine and Nervous System Disorders such as Multiple Sclerosis, Epilepsy and Alzheimer’s Disease.
- Digestive disorders including Crohn’s Disease, IBS and Ulcerative Colitis.
- Injuries from accidents that cause fractures, burns and brain injuries.
This is far from an exhaustive list; consult your policy, insurance company, or a disability lawyer if you’re unsure whether your condition is covered.
There is a Waiting Period Before You Can Qualify for Long-Term Disability
Aside from suffering from a disabling condition, one of the first criteria in qualifying for long-term disability is that you must complete a waiting period before you are allowed to file a claim, and you must be disabled for that entire length of time.
This is sometimes referred to in an LTD policy as an ‘elimination period’ or ‘qualifying period’ (your policy may use a different name). It can be approximately 60 to 180 days, which means that there will be a significant amount of time when, because of your disability, you will be unable to work and receive pay.
Finding Financial Support During the Waiting Period
The chances are that even if your employer provides paid sick days, they will likely run out during the early onset of your disability and long before you are eligible to qualify for LTD benefits. Employers and workers sometimes also purchase short-term disability insurance for this very reason.
Short-term disability (STD) coverage is designed to provide temporary financial support during a brief illness or disability. Accordingly, it also takes a lot less time to apply for and receive short-term disability benefits because claims are faster to process. Short-term disability benefits expire much sooner than LTD coverage, but they may provide a higher percentage of your employment income. Find out more about short vs. long-term disability.

Employment Insurance (EI) Sickness Benefits and CPP/QPP
The Government of Canada’s Employment Insurance (EI) sickness benefits can provide qualified workers with payments of 55% of their pre-disability earnings to a maximum of $650/week. New claims established on or after December 18, 2022, are eligible for a maximum of 26 weeks of benefits. If your medical condition prevented you from working prior to that date, you are only eligible for the previous maximum of 15 weeks.
You can apply for EI sickness benefits after being medically absent from work for at least a week, and your earnings have decreased by at least 40% as a result. This provides a person waiting to qualify for long-term disability or those who don’t have STD or LTD coverage with a means of financial support. Canada Pension Plan (CPP) disability benefits and Quebec Pension Plan (CPP) disability benefits are also potential sources of income replacement for those without long-term disability insurance or in addition to LTD coverage.
Depending on your policy, you may have to repay EI benefits if you begin receiving benefits before qualifying for LTD or STD benefits, or your insurance company may simply reduce your payments by those EI or CPP/QPP benefit amounts.
Filing a Claim – What to Include in Your Application to Qualify for Long-Term Disability
An application for LTD benefits contains three sections, often referred to as statements, that are required from at least three parties:
- The Insured (Plan member/ Employee) – In this section, you describe the specifics of your duties at work, your diagnosis, how and when your disability and its symptoms prevented you from working, and what you’ve done regarding treatment, among many other questions.
- Treating Physician – Your doctor will have to include all relevant notes, charts, reports, tests, etc., that support your claim for disability benefits.
- Your Employer – A manager or supervisor will be asked to answer questions regarding your role, pay, performance, potential conflicts and other workplace information that may be related to your disability.
The Importance of Medical Evidence to Support Your Claim
It’s vital for the success of your claim to prove that you qualify for LTD benefits by backing up your and your physician’s statements with medical evidence for disability claims. Insurance companies usually insist that verifiable, non-subjective evidence like blood tests and diagnostic imaging should be included with a claim for it to qualify for long-term disability benefits.
This means that you must be completely honest with your treating physician about your symptoms so that they can better understand the specifics of how your condition affects you and how it has manifested in you. Patients diagnosed with the same condition can often experience different symptoms and may have developed the condition in separate ways. This can lead your physician to order different tests and treatment plans to address the root concerns that result in more effective care.
But it is also crucial that the documentation your treating physician attaches to their statement is accurate and consistent with your statement and that your treatment plan makes sense. (You must also comply with all aspects of your treatment plan for your claim to have a chance of approval.)
Insurance companies are in business to make money. They do this by denying claims even if they don’t have solid grounds for doing so. They will scrutinize every assertion in your claim, and if they find an inconsistency between what you’ve stated and the information in your physician’s reports, the tests ordered, the treatment plan or anything else, your claim will probably be denied.
Medical Evidence and Mental Health LTD Claims
LTD benefits can be challenging to get approval for mental health disability claims and other “invisible illnesses” like chronic pain and fatigue syndrome, fibromyalgia and traumatic brain injuries where the illnesses/injuries can’t be proven with a blood test or diagnostic imaging because they don’t appear in any current testing procedures.
This does not mean that claims for these illnesses and injuries are illegitimate or impossible to get approved. They are covered conditions in many LTD policies and have been widely recognized as legitimate disabilities.
If a claim for a mental health disability is denied, insurance companies will often rely on the “lack of medical evidence” reason for the denial because it sounds like a policy rule. They are hoping that the claimant will figure that their hands are tied and walk away. Unfortunately, this happens far too often.
The truth is that a “lack of medical evidence” decision in these cases is not a valid reason for denial on its own. If your claim for LTD benefits was denied for this reason, or any other, speak to a long-term disability lawyer right away. They may be able to get you the benefits you deserve regardless of what the insurance company says in the denial letter.


0 Comments